This is part 2 of a series that deals with Stress and Addiction. It one part of a multi-part series of posts in which I attempt to provide a detailed analysis of all facets of one the most important questions in the addiction field: Why does one person become and an addict and another does not?
In Part 1 I showed how some forms of stress used in the laboratory, tail-pinch and social-stress, were able to increase the amount of psychostimulants self-administered by rats. Let’s expand this discussion to consider stress that may have parallels in human society.
Note: It is important to keep in mind that l am not making the claiming that stress exposure is the cause of addiction. I am merely providing evidence that your environment, specifically stress exposure, can increase your susceptibility to becoming an addict.
Can stress during childhood effect your susceptibility to becoming a drug addict?
It’s an intriguing question with many societal implications, given the disparities in the environments that children from different socio-economic backgrounds experience in the United States (I recommend reading Jonathan Kozol if you’re interested in learning about these disparities). But I’m not a sociologist, economist, public policy expert, etc. so I’m not capable of giving you my professional opinion on all the facets of this complicated issue but I can discuss the science behind the effects of early-life stress on drug-taking behavior.
Paper #1
This first paper looks at rats and the effects of stress during very early life on self-administration of cocaine as an adult but first, a little primer on the rodent life cycle. Rats and mice are mammals and like all mammals, give birth to live young. Litter size can be anywhere from 4-8 depending on the strain of animal. Animals born in the same litter are called littermates (note: this term doesn’t really have a human equivalent since humans typically only give birth to a single child at a time. Though we do have the terms twins, triplets, etc.).
Newborn animals (including humans) are called neonates. The mother rodent will then nurture her pups but feeding them breast milk through her nipples. All mammals are raised in this manner (even whales). This generally occurs for about three weeks in mice. In the lab, pups are then separated from the mother by the scientist, so they can become acclimated to an adult diet (i.e. not breast milk) but naturally, young mice will stop drinking breast milk once they are old enough The process of switching from breast milk to solid foods is a called weaning. Rodents are still considered in the adolescent stage for another three weeks after weaning. They go through puberty—the biological process in which mammals reach sexual maturity—at about 6-7 weeks of age and are then considered adults. *Note: these approximate times are for mice. Rat stages fall a little later.
The first study stresses rats during the neonatal phase by handling the newborn pups and separating them from their mother for 1 hour a day for days 2-9 after the date of birth. The authors call this neonatal isolation stress. The rats are then allowed to reach adulthood. At day 100 (3 months after the end of neonatal isolation stress) the stressed rats and rats from the same litter that were not handled (control group) underwent catheter implantation surgeries and then were tested for acquisition of cocaine self-administration for several didn’t doses.
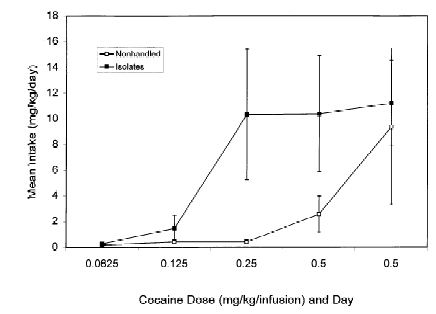
Interestingly, as shown in Figure 1, the rats that underwent the neonatal isolation stress self-administered more cocaine at lower doses (0.125mg/nose poke) and 0.25mg/nose poke). However, this effect was not seen at a higher dose (0.5mg/nose poke). These experiments suggest that early life stress can have an effect on adult rats and increases the pleasure they get from the drug and makes them more likely to self-administer cocaine at a dose they otherwise might not be interested in. The self-administration data are summarized in Figure 2.
What’s really fascinating is how a relatively brief period of stress (1hr a day for 7 days) can have such a drastic effect on the rats’ behavior 100 days later! This study suggests that stress during early life can have permanent (or at least, very long lasting) effects on brain function.
Paper #2
 The second study takes a similar approach but looks at different developmental time period. This study isolates rats (meaning rats are placed in individual cages rather than with their littermates) during adolescence, days 24-42 after birth (the experimental group, ISO). The control animals were socially housed during this time (SOC). This time frame falls after weaning but before puberty. On day 43, ISO animals were than housed together and a few weeks later, at 12weeks of age (well into adulthood) ISO and SOC rats were tested for self-administration of cocaine.
The second study takes a similar approach but looks at different developmental time period. This study isolates rats (meaning rats are placed in individual cages rather than with their littermates) during adolescence, days 24-42 after birth (the experimental group, ISO). The control animals were socially housed during this time (SOC). This time frame falls after weaning but before puberty. On day 43, ISO animals were than housed together and a few weeks later, at 12weeks of age (well into adulthood) ISO and SOC rats were tested for self-administration of cocaine.
Similar to the other study, the authors found that isolated rats acquired cocaine self-administration at a low dose of cocaine (0.0625mg/nose poke), which means that animals that underwent the social isolation stress self-administered more cocaine at a low dose when compared to the socially housed control animals. This is seen in the left half of the graphs in Figure 1 (the left panel shows nose pokes while the right panels shows the total amount of drug self-administered). However, at a higher dose of cocaine (0.25mg/nose poke), the right half of the graphs in Figure 1, there was no difference in self-administration between the two groups.
Importantly, the isolation stress also had an impact on motivation to take the drug. In the next experiment, rats were tested on a progressive ratio self-administration where they have to nose poke multiple times in order to get a single dose of drug. The number of pokes required increases everyday until the rat is no longer willing to try to get the drug. This limit where the animal gives up is called the break point and it is a measure of how hard the animal is willing to work to get the drug (ie how motivated is the animal for the drug).
As you can see in Figure 2, rats that underwent the social isolation stress during adolescence had higher break points, which indicates they were willing to nose poke more times in order to get the drug (more motivated).
In summary: these experiments also showed that stress that occurs early in the rats life (during adolescence) can have a long lasting impact on the rat brain. The stress made the rats more likely—more susceptible—to acquire self-administration behavior. That is to say, early life stress caused the drug to appear to be more pleasurable to those animals (they wanted to self-administer more of the drug) than for the control, socially housed animals.
In conclusion, these papers have shown that, in rats, stress during early life can have significant effects on an animal’s susceptibility to becoming an addict. Many other papers have identified similar findings. As I alluded to at the beginning of the post, this knowledge has disturbing implications for humans raised in drastically different environments.
However, let’s briefly discuss some caveats to these studies. You are probably wondering, “well, that’s good and well for rats, but has this effect been proven in humans?” First, one of the reasons we run these types of experiments in mice and rats because it is much easier to control for all the other variables that would make interpreting the experiment extremely difficult. Fortunately, we can’t take a bunch of kids, stress them out during their childhood, and then see how much drugs they take at as an adult! But there are other types of analyses and experiments that could be run using data gathered from the “real” world.
Are there studies in humans that confirm the animal studies, that early life stress can increase the susceptibility to addiction?
The answer is yes! Lots of them! I don’t have time to review them all but thankfully many other scientists have. Check out these two review papers for a summary of some these studies. If you are interested in stress and addiction studies in humans, please let me know! I would be happy to devote a post or two to this topic.
Finally, I would just like to end on a broader point, these studies once again confirm how brain development during early life can have far-reaching effects on adult hood (many other fields look at the general top of early life brain development). Indeed, the conditions under which we are raised are an important contributor to how we turn out as adults. But let’s not forget the role of genetics (this will be saved for a future discussion)!
Next post I’ll wrap up the Stress and Addiction discussion by looking at some of the molecular details of how and why stress increases susceptibility to addiction.
Thanks for reading!