At this point, I would think that knowledge about the vastness and seriousness of the prescription opioid and heroin epidemic, the biggest threat to American health and well being since the HIV/AIDS epidemic, would be common knowledge. Of course, given the abundance of shiny Internet things to tantalize easily distracted Americans, this is unfortunately not necessarily the case. Thankfully the New Yorker, with their characteristic excellence in reporting, has just released a superb and humanizing article on the opioid epidemic in their June 5 & 12, 2017 issue.
Read the article here.
The piece puts a much-needed human face to the horrors and misery of opioid addiction and the too-frequent death by overdose. Margaret Talbot, the article’s author, zeroes in on Berkeley County, West Virginia, in the heart of a region of the country hardest hit by the epidemic. I don’t want to give away much (because you should actually just read the article) except that the stories are heart wrenching yet balanced, and thorough in way that only the New Yorker can deliver. While the article is largely about the lives of people affected by and fighting against the epidemic, I was disappointed with a couple of points that were either made incorrectly, weakly, or not at all.
First, the article barely talks about how the epidemic arose in the first place. It mentions Purdue pharmaceuticals, the bastards behind Oxycontin (drug name: oxycodone), and that prescription opioid abuse led to heroin addiction but does not describe how the surge in addiction to prescription opioids occurred in the first place. The article describes the main problem with Oxycontin is that it can be crushed and snorted but a 2010 formulation of the drug reduced this risk. While this is indeed true, the article neglects to mention that when someone is first prescribed an opioid like Oxycontin for chronic pain (as was the case in the late 90s and early 2000s despite any evidence for the effectiveness of opioids in the treatment of chronic pain), the addictive potential of opioids often led to opioid substance abuse disorder in people who took it as prescribed (see this comprehensive article for more info). This is the big point, many of the people that eventually abused opioids started down that road by taking the drug as prescribed! Talbot incorrectly frames the big picture problem but she then goes on to correctly describe how those addicted to prescription opioids found their way to the cheaper and more abundant heroin.
The article goes on to mention the CDC’s release of guidelines on opioid prescription but fails to cite that this guidance came out as late as March, 2016, well after the epidemic had already taken root and thousands were already addicted and dying of overdose (I wrote an article on the CDC’s guidelines last year and highly recommend you read that article too if you want to learn more). The CDC’s guidance is mainly about the point I made above, that the over-prescription of opioids is the real cause of the epidemic, not just the crushable version of Oxycontin, and the limitation of opioid prescription is one of the huge policy interventions that is needed.
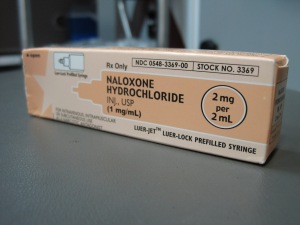
Later in the article, Talbot introduces us to Dr. John Aldis, a retired U.S. Navy Physician and resident of Berkeley County, WV who took it upon himself to educate people on how to use Narcan (generic drug name: naloxone), the treatment for opioid overdose. Dr. Aldis makes the critical point about the importance of medication-assisted treatments such as Suboxone (generic drug name: buprenorphine) and methadone. I appreciated the point made in the article that some patients may need these vital treatments long-term, or even for life, to combat the all-consuming single-mindedness of opioid addiction. However, beyond this passing mention, I felt that medication-assisted treatment was only weakly covered. There is still a great deal of ignorance about these treatments. Indeed, current HHS secretary Tom Price falsely characterized them as “replacing one opioid with another” and was majorly criticized by addiction experts. The reality is that there is overwhelming scientific evidence (I’ve written plenty on this site) describing the effectiveness of methadone and buprenorphine at 1) keeping addicts off of heroin, 2) allowing them to be able to live their lives without suffering from withdrawals and cravings, and 3) most importantly, keeping them alive. Talbot could have done a much better job of really hammering these points home but she seemed reticent, for some reason, to discuss it in detail in this article.
Finally, the article repeatedly emphasizes the importance of rehab clinics and tells the story of a huge victory for Martinsburg, WV (a town in Berkeley County) when the city council agrees to open a clinic in the town itself. I do not want to discount the importance of an addict assessing their addiction and taking an active role to end it, but this article does miss another critical point: rehab clinics only exist because addiction medicine is not part of medical school curricula and most hospitals are ill-equipped to treat those suffering from addiction. I feel this article could have really made the case for the importance of training for doctors in addiction medicine and the necessary shift that needs to happen for addiction treatment, a move away from overpriced (and often ineffective) private rehab facilities, and to public hospitals. Unfortunately, this point was not made.
Despite these missed opportunities, I commend Talbot and the New Yorker for a well-written article and thank them for this important piece that I encourage all to read.